Hey there Guys,
Today I thought I would introduce the topic of prostate health. The prostate is an important gland for men and sexual their function, however disease of the prostate impacts on a man’s ability to urinate. Problems with the prostate can be broken down into three main areas, infection and inflammation, enlargement, and cancer. Today I’ll cover each of these topics. Before we do though let’s talk a little about the prostate gland and what it does.
What is the prostate?
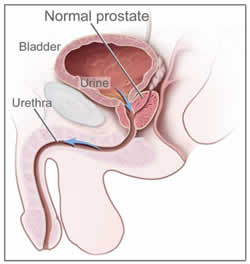 The prostate is a gland in males that sits just under the bladder. Its job is to secrete alkaline fluid into the ejaculate or “cum” that helps protect sperm from the acidic environment of the vagina.
The prostate is a gland in males that sits just under the bladder. Its job is to secrete alkaline fluid into the ejaculate or “cum” that helps protect sperm from the acidic environment of the vagina.
The prostate is around the size of a walnut at puberty and is shaped like a doughnut. Through the centre of the doughnut is the urethra, the tube that empties the bladder through the prostate and down to the penis. The prostate slowly grows as men age under the exposure to testosterone from the testes.
Because of its position just under the bladder the prostate can actually be felt via the anus. If you slide a finger into your anus you can feel the prostate; it’s a smooth walnut shaped gland lying on the upper side about the length of the index finger deep.
Because of the prostate’s proximity to the bladder, prostate problems normally cause symptoms associated with passing urine.
One of the most common prostate problems is inflammation, known as prostatitis.
What is prostatitis?
Prostatitis is when the prostate gland has become inflammed. This leads to symptoms with urination in particular:
- needing to pass urine more often
- pain when passing urine
- poor urinary stream
- the sensation of needing to pass urine despite having just gone
- dribbling of urine after going to the bathroom
- sometime there can be pus or blood in the urine
- pain in the groin
- in extreme cases there can be fevers and chills
Prostatitis is quite common with about one in eight men suffering with the symptoms at some time in their life. The good news is that while it can be very uncomfortable it is rarely life threatening. If you are having extreme pain, fevers or are feeling very unwell, it’s important to see your doctor as soon as possible.
In many cases prostatitis is caused by bacteria that has passed up via the urethra. This can lead to infection of the prostate gland, urethra and sometimes the bladder. The good news is that by explaining your symptoms, and with a straight forward examination by your doctor, you are normally able to start antibiotic treatment. As part of your examination your doctor may need to pass a finger into the bottom to feel the prostate gland.
After your exam it can be helpful for two samples of urine to be collected. One is the first part of urine that comes out of your body and the second, the next part of urine to come out of your body. These samples are sent to be checked for bugs that commonly cause prostate inflammation, in particular chlamydia, gonorrhoea, and few other bugs that are sometimes found in the gut.
There are some cases where, despite testing, no bacteria are able to be found. It’s a bit of medical mystery what causes the inflammation in these cases however treatment with anti-inflammatory medications and medicines that make passing urine easier can sometimes help.
In rare cases prostate inflammation can last a longer period of time, so it can be worth discussing with your doctor a review with an urologist or specialist in men’s health.
 For a great print out on prostatitis from Andrology Australia, please click here.
For a great print out on prostatitis from Andrology Australia, please click here.
What is benign prostatic hyperplasia?
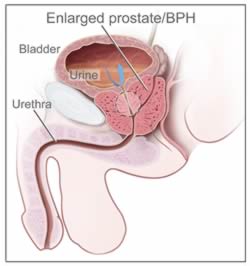 Benign prostatic hyperplasia, or BPH, is the medical name for prostate enlargement.
Benign prostatic hyperplasia, or BPH, is the medical name for prostate enlargement.
As men age the prostate gland continues to grow. Starting at walnut size at puberty the prostate doubles in size by the age of 50 and then doubles again by the age of 80.
The prostate gland is covered in a fibrous sheath, so as the prostate grows the tissue is forced inwards which narrows the urethra, the centre part of the prostate which allows urine to drain from the bladder.
This narrowing of the bladder outflow leads to the most common symptoms of BPH:
- difficulty starting urine flow
- needing to strain to pass urine
- decreased urine flow, “not being able to hit the back of the bowl”
- needing to pass urine more frequently
- needing to get up at night to pass urine
- dribbling after finishing passing urine
- urgency, the feeling of needing to pass urine even if urine was just passed
While the good news is that this problem is not life threatening, it can be very annoying. If left untreated it can lead to problems with the bladder and kidneys if extreme.
BPH is quite common with one in seven men suffering between the age of 40-49, increasing to about one in four men by the age of 70.
If you have been suffering any of the symptoms above it is worth discussing them with your doctor as there are some effective treatments available.
When talking with your doctor he will ask some quite detailed questions about your symptoms. As part of the physical exam he will need to pass a finger into your anus to feel the shape of the prostate and will normally organise a blood test called a prostate specific antigen test or PSA for short.
Part of the reasoning for doing this testing is to differentiate the symptoms of BPH from potential prostate cancer. If your doctor has any concerns he may choose to organise an ultrasound of your prostate to get an good idea of the shape and density of your prostate.
As mentioned there are a number of natural, medical and surgical options to treat prostate enlargement.
![]() For a fantastic summary check out this great resource from the guys at Andrology Australia.
For a fantastic summary check out this great resource from the guys at Andrology Australia.
Click here to download a fact sheet on BPH from Andrology Australia.
What is prostate cancer?
Prostate cancer is the most common cancer for men in Australia. Each year more then three thousand men die from prostate cancer, equal to the rate of breast cancer deaths in women.
Prostate cancer occurs when the cells of the prostate start to grown and divide in an unregulated way. This can lead to changes in the function and size of the prostate.
Thankfully prostate cancer is a type that tends to grow quite slowly and tends to stay within the prostate. A small percentage of prostate cancers can be quite agressive that tend to present earlier, grow faster and spread to other parts of the body.
Recent research has shown that the gene associated with breast and ovarian cancer (BRCA1&2) is also associated with aggressive forms of prostate cancer. Because of this, a family history of prostate cancer or breast and ovarian cancer associated with the BRCA gene are considered significant risk factors for prostate cancer.
The main risk factor for prostate cancer is age which is why The Prostate Cancer Foundation of Australia recommend considering screening for prostate cancer starting at age 40 if you have a significant family history or from 50 if you do not.
Prostate cancer screening in men who are symptom free is a difficult topic, as recent studies have shown that increased screening can lead to excessive and invasive procedures that may not have additional benefit. Because of many factors it is the position of Andrology Australia, The Royal College of General Practitioners in Australia and the Urological Society of Australia and New Zealand that testing should only be done after a detailed discussion with your doctor about the pros and cons of testing, your current risk of prostate cancer and most importantly your concerns.
There is a great site by the Lions Club Australia and discusses the pros and cons of prostate testing and has fantastic advice and information.
Lions Australia Prostate Cancer Website.
If you have a strong family history such as a father or brother with prostate cancer, or a mother or sister with breast or ovarian cancer it’s important you discuss these issues with your GP to allow for informed choices when it comes to testing.
If you are suffering with any of the following symptoms testing is likely to be useful:
- difficulty passing urine, in particular starting or stopping the stream
- poor urine stream (not hitting the back of the bowl)
- dribbling after passing urine
- not being able to fully empty the bladder or needing to get up frequently at night to pass urine
- blood or pus in the urine
- pain in the groin or pelvis
How is screening for prostate cancer done?
Screening for prostate cancer is a fairly straight forward process.
First your doctor will discuss with you your current symptoms and concerns. Feel free to get down to the nitty gritty, this is important information and is very helpful in letting your doctor know what to consider.
Next your doctor will discuss getting screening testing done and whether it is appropriate for you. If he or she considers it important the actual screening is quite straight forward.
First part of the test to examine your prostate is done by sliding a finger into the anus. The prostate can be felt about a finger length in. During this test we are feeling if the prostate is soft, symmetrical and smooth (which are good things) or hard, lumpy or asymetrical (these are not good things).
The second part of the screening test is to get a prostate specific antigen (PSA) test. This is a simple blood test and you do not need to be fasting to have it done.
Two important things to note:
Firstly, you need to have both parts done, you can’t have one without the other.
Secondly if either are abnormal you may require additional testing to formally check for prostate cancer. This is done via ultrasound where small samples of prostate tissue are taken via biopsy to look at them under a microscope. If your doctor feels this needs to occur he or she will be able to refer you to see a urologist, a specialist doctor who looks after prostate health who can help you make the decision on what to do and help guide treatment if needed.
To learn more about prostate health.
If you are interested in learning more about prostate health here are some great resources you might find helpful:
The Prostate Cancer Foundation Of Australia
The Urological Society Of Australia and New Zealand’s prostate health page
Andrology Australia’s page on prostate health
The Better Health Channel’s page on prostate health
On a final note…
If you or a friend are living with prostate cancer there is some great news. The Prostate Cancer Foundation of Australia has started a pilot program to help support gay and bisexual men. With over twenty thousand Australian men diagnosed yearly it’s great new to hear that there is going to be a voice and support for the gay men who are diagnosed. If you would like to learn more be sure to check out the press release at Prostate Cancer Foundation of Australia:
“Better Prostate Cancer Support For The Gay Community”
Wow that one was a marathon! Thanks for sticking with me.
Of course if you have any questions please feel free to contact me by leaving a comment, an email or making a one-on-one appointment at my practice. I’ll do my best to make sure you get the best advice.
If you have found this helpful please hit the like button below to help get the word out, it really helps!
Yours in good health, and may you pee freely!
Dr George

Benjamin Andrews says
I found it interesting that you state that you can’t have one part of the test without the other. My dad is at an age where he needs to get yearly checks for cancer. I will keep this mind while we look for a prostate clinic that we can take him to.
George Forgan-Smith says
yes! Please do ensure he gets a comprehensive discussion as well as examination. Often it’s in what the patient tells us that can lead to the diagnosis.
I had one patient who just had a single liver enzyme that was high that indicated something was going on.
Dr George